Your Back Isn’t Broken — Your Nervous System Just Thinks It Is
At some point, you probably learned you should be afraid of hurting your back.
Not because your spine is actually fragile (because it isn’t). And not because your back is poorly designed (because that isn’t true, either). But because the narrative in the late 1990s and early 2000s was that your spine was something you should protect at all possible costs.
I used to feel this way. I started my career during the heyday of Swiss ball training, transverse abdominis activation, and laboratory research that was assessing when a pig’s spine buckled under load. It was the body fragility era and it was having a moment.
I initially bought in. I had clients breathing into blood pressure cuffs before lifting weights. I was meticulous about “appropriate spinal stiffness.” The appropriate spinal stiffness was necessary for “optimal spine alignment.”
Or so I was told.
And then I started paying attention to what was actually happening, in the research, and in the room with my clients. I ditched the blood pressure cuff, but kept the stability ball, because who doesn’t like playing on a giant ball?
Fortunately, the science has largely caught up. Body fragility gave way to body resilience. But here’s the thing about fear: it’s a stubborn input. Once you believe your back is something to protect, that belief doesn’t evaporate when the research changes. It lives in how you move. I still see it. It’s the person who holds their breath before bending over or the guarded way someone describes picking something up off the floor. It’s the low-grade vigilance that follows a person long after the original pain is gone.
This post is about changing that input. Because the spine isn’t fragile. And once you actually believe that, not just intellectually, but in the way you move through a Tuesday, everything shifts.
This is especially common in people who are otherwise fit and active — people who run, lift, do yoga, and still can’t shake the sense that their back is the weak link. If that’s you, the issue is almost certainly not structural. It’s that somewhere along the way, you learned to treat a part of your body as a liability, and that belief became a pattern. Movement can change the pattern. But first you have to change the very first input — the belief.
What your spine is actually built to do
Is the spine actually fragile?
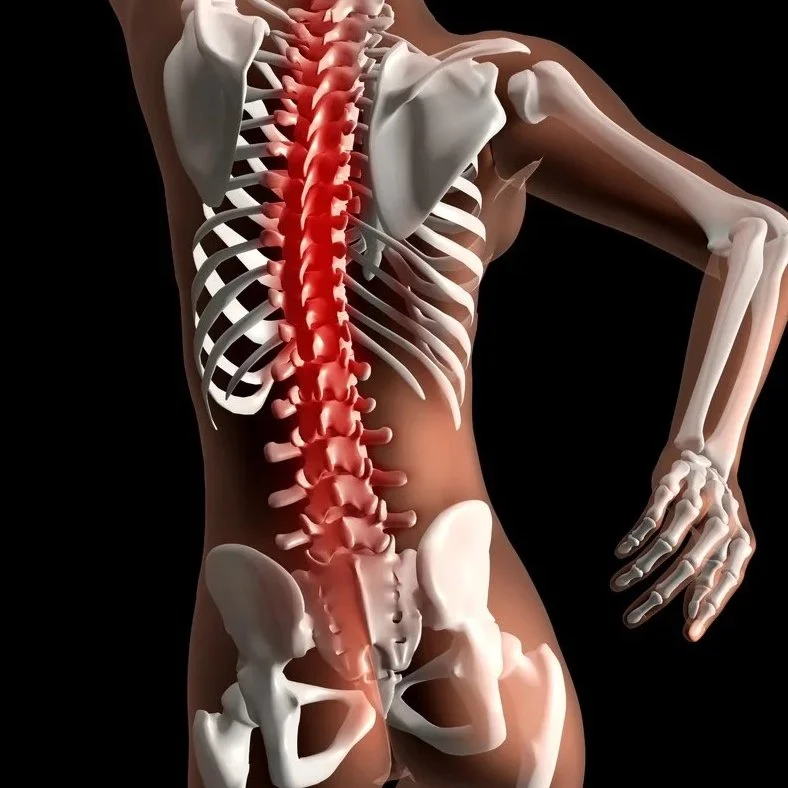
No — and the anatomy makes this clear. Here’s what’s actually going on inside your back:
Between each segment of your spine are strong ligaments that prevent each vertebra from excessive movement. In addition to the ligaments, layers of muscles in the front and back allow your spine to pitch forwards and backwards, tilt side to side, and rotate. Most movement is a combination of at least two of these things.
Between each vertebra you have a disc. It consists of a strong outer shell and an interior that is soft and viscous, kind of like the inside of an egg. The disc provides cushion and acts as a shock absorber, like a pair of Hoka shoes.
Your body is a living, physiological structure. It’s constantly changing. The inside of the disc can push through cracks in the outside of the disc, oozing outward. But not always, and not forever.
Because you are a living structure, most injuries heal. Even disc material that oozes outward can stop oozing. The body is not a machine with parts that break and stay broken.
Articles that make bold claims like “research says this exercise is bad for your back and this exercise will fix your low back pain” should be treated with a healthy dose of skepticism. Whatever claim you want to make, there is likely a study that supports it. High-quality research on exercise and low back pain is genuinely hard to do.
Lifting something relatively light with a rounded back won’t cause anything to implode. In fact, you probably do this without thinking about it regularly. When you lift something heavy, rounding the back does increase compressive stress on the spine, which is worth knowing. The principle: different load, different strategy.
On aerobic exercise and low back pain: A recent meta-analysis of 17 studies and 1,146 participants found that aerobic exercise helped with low back pain — but only when performed more than 5 days per week for more than 3 months. Aerobic exercise combined with other exercise produced significantly better outcomes than aerobic exercise alone (Sany et al., 2023). Movement helps. Consistent, varied movement helps more.
Basically, movement makes most things feel better, including your back. But you probably know that already. Otherwise you wouldn’t be reading a 2,000-word post on why the spine isn’t fragile.
Why believing your back is fragile changes how you move
Why does fear of back pain change how you actually move?
The short answer: because the brain processes beliefs about your body the same way it processes everything else: as inputs that shape movement output. And the neuroscience behind this goes back further than you might expect.
Way back in the late 1800s, the world of neuroscience was having a moment. Researchers in Europe and the US were mapping how the nervous system worked, and movement was at the center of the debate.
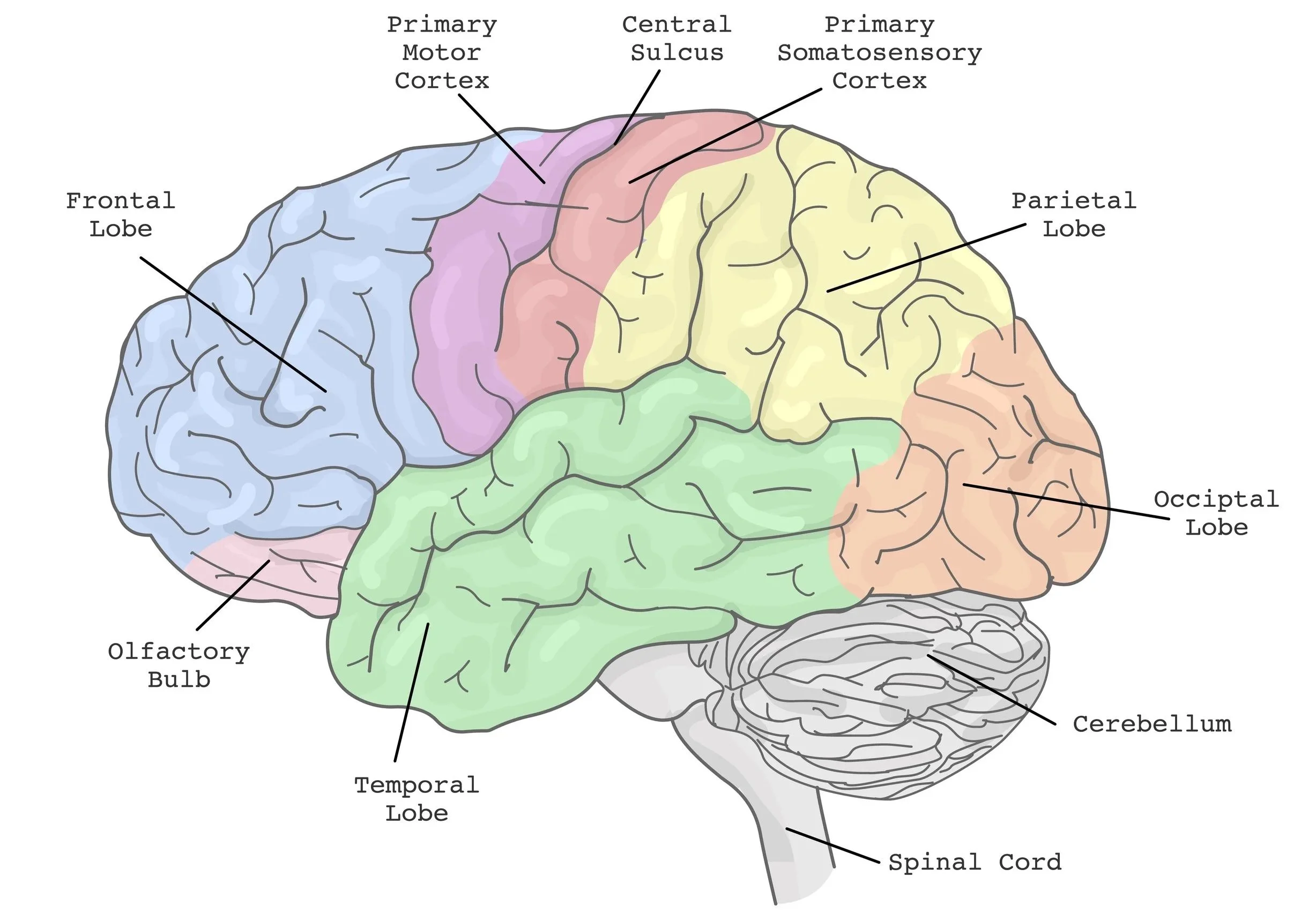
In one camp was Hughlings Jackson, an English neuroscientist credited with saying that “the nervous system knows nothing of muscles, it only knows of movements.” He believed the motor cortex, the part of the brain that executes movement, represented whole, functional movements rather than individual muscles.
A short while later, a neuroscientist named Charles Sherrington did numerous cortical mapping studies on primates, stimulating parts of the brain and observing which body part moved. What he observed were movements that were fractional; by themselves they were small and uncoordinated, but regularly integrated into larger movements.
Sherrington’s student, Wilder Penfield, picked up where he left off, mapping the human brain’s motor responses using low-level electrical stimulation. Unlike Jackson, Penfield believed movement was an integration of memory, reason, and sensory information — and that the brain orchestrates which pieces of you coordinate to produce the movement you want.
We’ve learned a lot since then. We know the brain thinks in terms of movement. We think in movement language all the time: jump for joy, race to the finish, whirling dervish. And at some level, the brain understands individual muscles too.
So what does this have to do with your back?
The way your brain processes information about your body is similar to the way it processes everything else — as a collection of inputs that produce an output. The output, in this case, is movement.
If you hold on to the belief that your spine is fragile — because someone told you your transverse abdominis doesn’t fire right, or your left internal obliques are weak, or your hamstrings aren’t strong enough — that belief becomes an input. And inputs shape outputs.
How you think about your body changes how your body moves. This is not metaphor. It’s neuroscience.
Which means all of that chatter about weak, misfiring muscles contributing to spinal fragility isn’t just unhelpful. It’s working against the very thing it claims to help. It doesn’t serve how you move. What it does, in my experience of working with clients across 24 years, is hold you back.
How to actually change the pattern
If you don’t have back pain right now
Keep doing what you are doing. If someone tries to tell you a muscle isn’t firing properly, smile politely and go about your business. I have had well-meaning massage therapists tell me all kinds of things about which muscles are or aren’t working. I smile politely and nod when appropriate, and then keep doing what I am doing, which has kept me pain free, running, and flipping upside down for 15 years. A practitioner making assessments based on how you look lying on a table is working with very different information than someone watching you actually move.
If you do have back pain that comes and goes (or mostly stays) — start here
Consider your patterns. We are efficient by nature. We find efficient ways to do everything: drink a glass of water, pour from a pitcher, climb stairs. When we do something for a long time — sit, stand, chop vegetables — we settle into the most efficient version our body knows.
Have you ever had your leg fall asleep because you stayed in one position too long? You shifted, the numbness went away, you moved on. That’s an extreme version of what I’m describing, with one key difference: the leg-falling-asleep sensation is a loud input that demands your attention immediately. A lot of the time, the signal from a repetitive position is much quieter. You don’t notice the discomfort until it’s no longer a soft whisper. It’s more like a wailing toddler.
Aerobic exercise is rhythmic, continuous, and naturally releases hormones that dull pain. When you combine that with movement that requires attention and body awareness, you build new patterns. The nervous system updates. The output changes.
Where I start with almost every client
These four steps make a significant difference in how people move, and they’re the foundation of the work I do:
Improve awareness of different parts of the spine
Improve awareness of what and how you are connected to the ground — through the feet if you are standing, pelvis if you are sitting, hands and knees if on all fours
Notice how you weight shift
Practice weight shifting with specific focal points in mind
They sound simple. They are not always easy. But they work consistently, because they change the inputs.
The video below shows these concepts in action.
The bottom line
After 24 years of watching people move, and the better part of a graduate education spent studying how the nervous system actually works, here is where I land:
The spine is not fragile. It is strong, adaptable, and extraordinarily well-designed for a life that involves bending, lifting, rotating, and occasionally picking things up off the floor in positions that would make a biomechanics textbook wince. The fear that surrounds it — the breath-holding, the guarding, the hypervigilance — costs more than it protects.
Changing that fear isn’t a matter of willpower. It’s a matter of input. New movement experiences, practiced with attention, create new patterns. The nervous system updates. The output changes.
If you want to understand more about how nervous system patterns show up in the way you move — and what to do about it — this is exactly what Spinal Intelligence is built around. It’s the framework I’ve developed over two decades of hands-on coaching, grounded in current neuroscience and written for people who want to understand their bodies, not just be told what to do with them.
You can learn more about the book here.
Your back is not the problem. Let’s start there.
References:
Pinto et al. (2025). https://pmc.ncbi.nlm.nih.gov/articles/PMC12909609/
Gunderson et al. (2025). https://pmc.ncbi.nlm.nih.gov/articles/PMC12591051/
Sany et al. (2023). https://pmc.ncbi.nlm.nih.gov/articles/PMC10579857/
Ward, N. The motor cortex and voluntary movement. https://zinabward.com/Misc/WardMvM.pdf
Jenn Pilotti, M.S., is a movement educator and author of Spinal Intelligence. She works with intelligent, high-performing people at the intersection of neuroscience, somatic movement, and physical fitness. jennpilotti.com